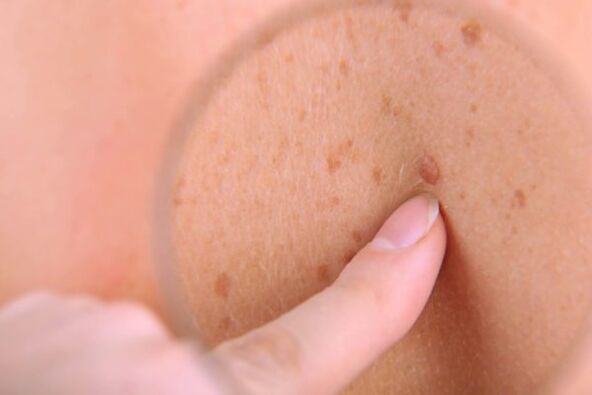
Reason for occurrence
- Congenital or acquired immunodeficiency;
- stressful situations;
- influenza;
- use of cytostatics;
- Long-term use of antibiotics, hormones, and non-steroidal anti-inflammatory drugs;
- Chronic vitamin deficiency;
- Persistent urogenital infection;
- Herpes virus is present in the body.

attention! The presence of HPV in the body does not guarantee the development of tumors.
risk subgroup
route of infection
- sexual. It is the most popular method of infection regardless of the type of sexual intercourse. The virus is also spread through kissing. Penetrates into the mucous membranes of reproductive organs and enters the body through microscopic damage. Infections can survive in them for a long time.
- During delivery. The infection occurs from mother to child during childbirth. At this time, the baby may develop oral genital warts and anogenital hyperplasia.
- domestic. It is rarely spread through contact. It enters the body through micro-tears in the skin. This happens when people share personal hygiene products.
Characteristics of papilloma
- Located in the body but no new growths are forming on the skin. In this case, doctors diagnose a hidden form of pathology. Pathogens without cutaneous manifestations can be detected using PCR;
- The virus grows on the skin in a free form;
- Promote epithelial cell degeneration from benign to tumor.
What do genital warts look like?
- broad, broad-based;
- Point to the thin stem. They often appear on the genital skin and armpits. Sometimes located at the corners of the mouth.
Symptoms and signs
- formation of growth;
- Skin allergies;
- Discomfort during sexual intercourse;
- Redness and itching.
attention! Skin irritation and itching sometimes indicate another condition. If such symptoms occur, you should consult your doctor immediately.
main difference
- Papillomas – round or linear with a thin base.
- Genital warts are irregularly shaped growths. Their uneven contours typically protrude 0. 5 cm from the skin.
diagnosis
- Vision test;
- PCR, which can determine the presence of HPV;
- Genotyping. Analysis to identify virus types;
- Histological diagnosis. Allows you to accurately determine the type of pathology and the likelihood of malignancy.
treatment method
- Take antiviral medications. This makes it possible to inhibit HPV activity;
- Improve immune system function - take vitamins and immune modulators.
Hardware removal
- surgical. Until recently, it was the main method of eliminating tumors. After the scab falls off, a scar will form on the affected area. This has prompted experts to look for other ways to remove the growth.
- Chemical. In order to burn off warts, special medicines containing strong acids are used.
- Freeze solidification. Freeze growth at low temperatures using liquid nitrogen. The increased risk of recurrence is a significant disadvantage of using this approach.
- radio waves. It's painless and quick.
- Use laser. One of the newest ways to get rid of skin growths. Not suitable for all warts.
possible complications
- formation of papillomas, genital warts, and warts;
- Papillomatosis. The tumor grows extensively;
- bleeding. Usually after excision of the papilloma with hardware;
- Infect. During oncological trauma, the likelihood of infection increases;
- Tumor suppuration;
- Ulcers form due to prolonged friction with clothing;
- Precancerous lesions;
- Cancer cell growth in the body;
- risk of skin cancer;
- Childhood suffocation. When the larynx is affected by papillomas, breathing difficulties often occur. There is a choking hazard.
important! Human papillomavirus is a serious pathology. It is impossible to ignore it and treat it independently. Otherwise, the condition may worsen.













































































